The Centers for Disease Control and Prevention (CDC) reported that roughly one in four older adults will fall each year, totaling about 36 million older adults who fall annually. But it’s important to understand that falling is not considered a normal or inevitable part of aging. While falls are nothing to take lightly, experts agree a fall (or multiple falls) is no reason to immediately pack up and head to a different home setting.
Brittany Ferri, a licensed occupational therapist with a background in geriatrics, said older adults who have fallen “will likely need some intervention, [such as] home modifications, rehabilitation, medication assessment/adjustments, but this doesn’t prevent them from living at home.” Falls at home may have a variety of causes and many of them are avoidable in the future.
What Are the Common Causes of Falling at Home?
The National Institute on Aging identifies a variety of potential factors for falling due to physical or health-related causes, home or environmental causes, or often some combination that falls under both categories. Before identifying common causes of falls (and how to manage or avoid them) to continue living safely at home, we do need to recognize that in some cases, staying at home may not be possible.
Conditions like advanced dementia or extreme frailty often require another environment, like a nursing home or care facility, especially if 24/7 home care isn’t an option. At the very least, there needs to be creative strategizing with a robust network of caregivers, noted Norman. Those cases aren’t the norm though, and most older adults who’ve experienced a fall can likely attribute it to something less extreme.
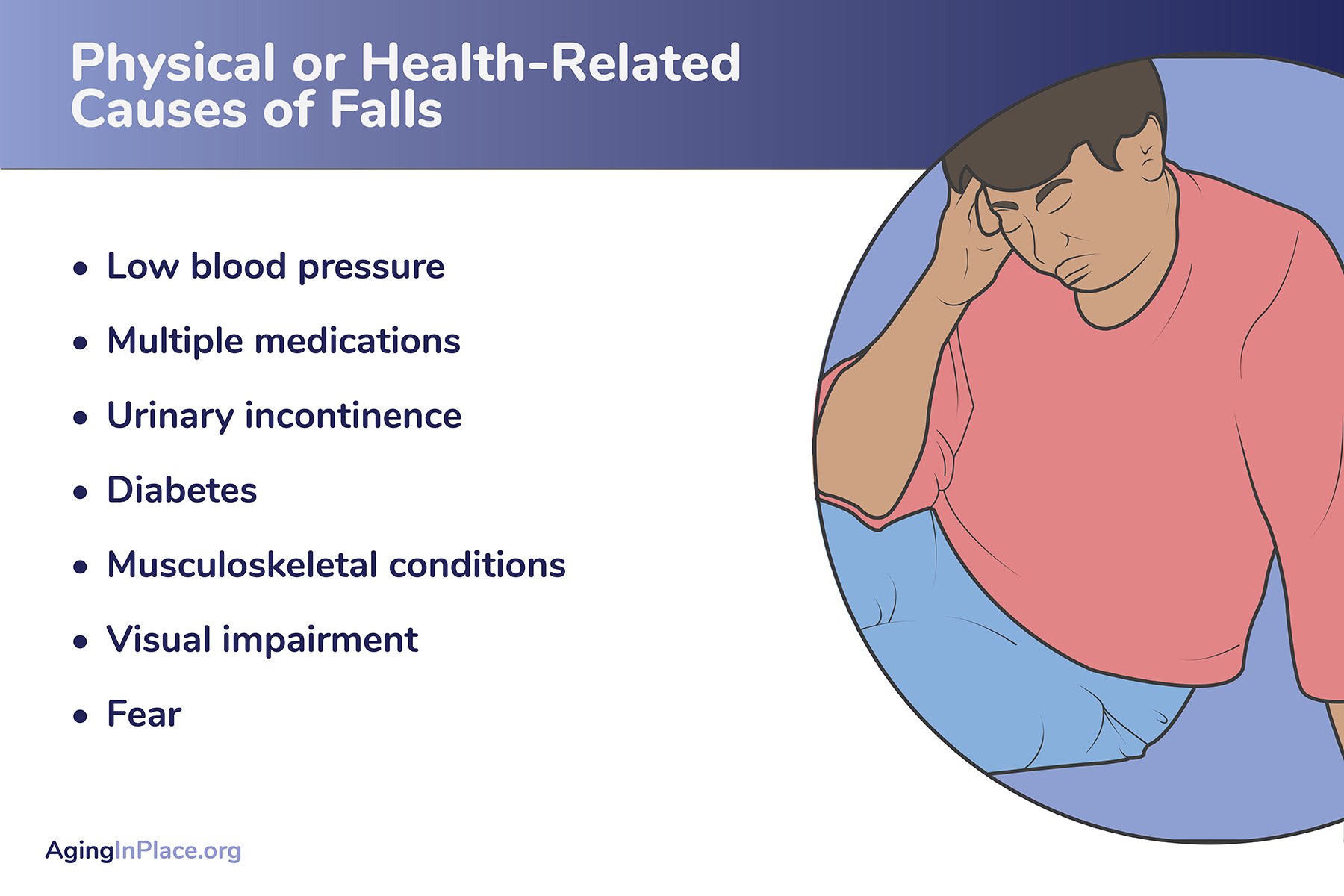
Physical or Health-Related Causes of Falls
Low blood pressure: Low blood pressure can cause symptoms like dizziness, light-headedness, and fatigue, all of which can contribute to falls by making someone weak and unstable on their feet. A sudden drop in blood pressure when going from sitting to standing, called orthostatic hypotension, is also a frequent contributor to falls. The Mayo Clinic identifies orthostatic hypotension as being particularly common in older adults.
Multiple medications: Multiple medications, also referred to as polypharmacy (which means taking four medications or more), increases the chance of side effects from medication interactions like dizziness, disorientation, confusion, and more that can cause falls. Unfavorable medication interactions are more likely to occur when an older adult is taking multiple prescriptions from multiple providers. Other prescribing doctors may not be aware of the patient’s exact prescriptions, resulting in inappropriate medication combinations. “Also, simply, the more meds a person takes (regardless of who prescribed them) the more likely there are to be unfavorable interactions,” added Norman.
Urinary incontinence: Urinary incontinence can lead to falls in a couple of ways. First, urinary urgency may cause an older adult to be less cautious as they rush to the bathroom, increasing the risk of falls. Second, if someone has a urinary tract infection that’s causing urinary frequency or incontinence, the infection itself may cause confusion and disorientation, particularly in older adults. Sudden confusion or delirium can be one of the earlier signs of a urinary tract infection in older adults, even before other symptoms like urinary discomfort are present. Excessive urination can also be a sign of diabetes, which is another potential cause of falls.
Diabetes: It’s common for people with diabetes to experience lightheadedness if their blood sugar dips too low, which can make them unstable and lead to falls. When left untreated or not well treated for a long time, diabetes also commonly causes neuropathy, which affects sensation in the extremities. Someone experiencing neuropathy in their legs or feet may not be able to walk safely, especially if there are rug corners, power cords, or other potential hazards in their path.
Musculoskeletal conditions: Sometimes falls can be caused by pain or stiffness in the joints, muscles, and bones. Conditions like osteoporosis and arthritis are well known for causing pain and impacting mobility. This pain can get worse during weight-bearing movement, particularly while on foot or transferring from one position or location to another. When pain or stiffness makes walking and transferring difficult, a fall can happen at any time.
Visual impairment: If an older adult has trouble seeing where they’re going, it’s not surprising that they may trip on uneven surfaces or bump into furniture. Even those who wear glasses may experience vision difficulties if their prescription is outdated or if they don’t wear their glasses consistently at home.
Fear: Unfortunately, the fear of falling can actually be a factor in causing falls to happen. Whether someone is fearful due to a previous fall or just because they know that falling is a possibility, older adults who are afraid of falling may be more unsteady on their feet as a result of trying to move too cautiously. People who suffer from anxiety can also experience symptoms that may cause them to fall, like lightheadedness, elevated heart rate, or blurred vision. Anxiety attacks and related symptoms can be triggered by a fear of falling, or even on their own without an obvious or related cause. “The No. 1 risk factor for falling is a history of falls,” added Norman.

Home or Environmental Causes
Area rugs: Area rugs are a common cause of falls in the home. Even though the height difference between a floor and a rug is typically pretty low, it’s enough for an older adult to catch their foot and lose balance—especially if an exposed rug corner has curled up, increasing the potential for tripping.
Slippery surfaces: This is particularly relevant in the bathroom, where anything from the floor to the toilet to the counter can be slippery. Slipping on wet floors in the bathroom is common, as are falls that happen when you try to grab something for balance or stability, like a counter, railing, or doorknob, and it’s slippery from moisture. While some may think adding a rug is a solution, the above section on area rugs clearly demonstrates that it is not a safer way to resolve the problem.
Clutter: Even though a floor may not look “cluttered,” anything that’s on the floor where an older adult may be walking is an opportunity to trip and fall. Objects like power cords can be particularly hazardous, as well as small items that move around the home like storage bags or boxes, pet toys (or pets themselves), pairs of shoes, or mobile electronics—like robot vacuums.
Poor lighting: Poor lighting particularly affects those who are visually impaired, but anyone can have an unexpected fall when an area isn’t well lit. Dim lighting makes it harder to see thresholds, clutter, and steps—and can make it difficult to assess distances.
Items out of reach: Attempting to access items that are out of reach can put you in an unbalanced position. Getting up on your toes or reaching with one hand can make you unstable, as can trying to balance on a step stool or other raised item.
Does Falling at Home Mean I Can No Longer Age at Home Safely?
In many cases, no. “Recurrent falls should mean that further investigation is required,” said Kimberly Smith, a doctor of physical therapy at Athletico Physical Therapy. “You need to take a closer look at the cause of the falls and understand what tools or assistance may be needed to help to decrease falls.” If you have family members or caretakers involved in your home and daily life, it’s a good idea to make fall prevention a concerted effort so that everyone is on the same page.
Sometimes a person’s physical condition can’t be improved or their home can’t be effectively altered to avoid falls, but most of the time there are steps that can be taken to reduce the risk of falling at home well before having to consider relocating.
“It is not an easy process to suddenly deem someone unsafe at home,” said Stephanie Ross, a licensed and registered occupational therapist. “Getting professionals involved who can help identify the cause is the best place to start, followed by making adaptations in their home and routines to best ensure their safety.”
Depending on who is involved in your current care, anyone from your primary physician to a physical therapist or other specialists may be helpful in creating the safest care plan and home environment.
Tip: A medical alert system with fall detection provides access to help if you fall or have a medical emergency. In fact, in an AgingInPlace.org survey, we found that out of the 1,000 medical alert users who responded, over 90% felt more confident in their daily lives due to the devices.
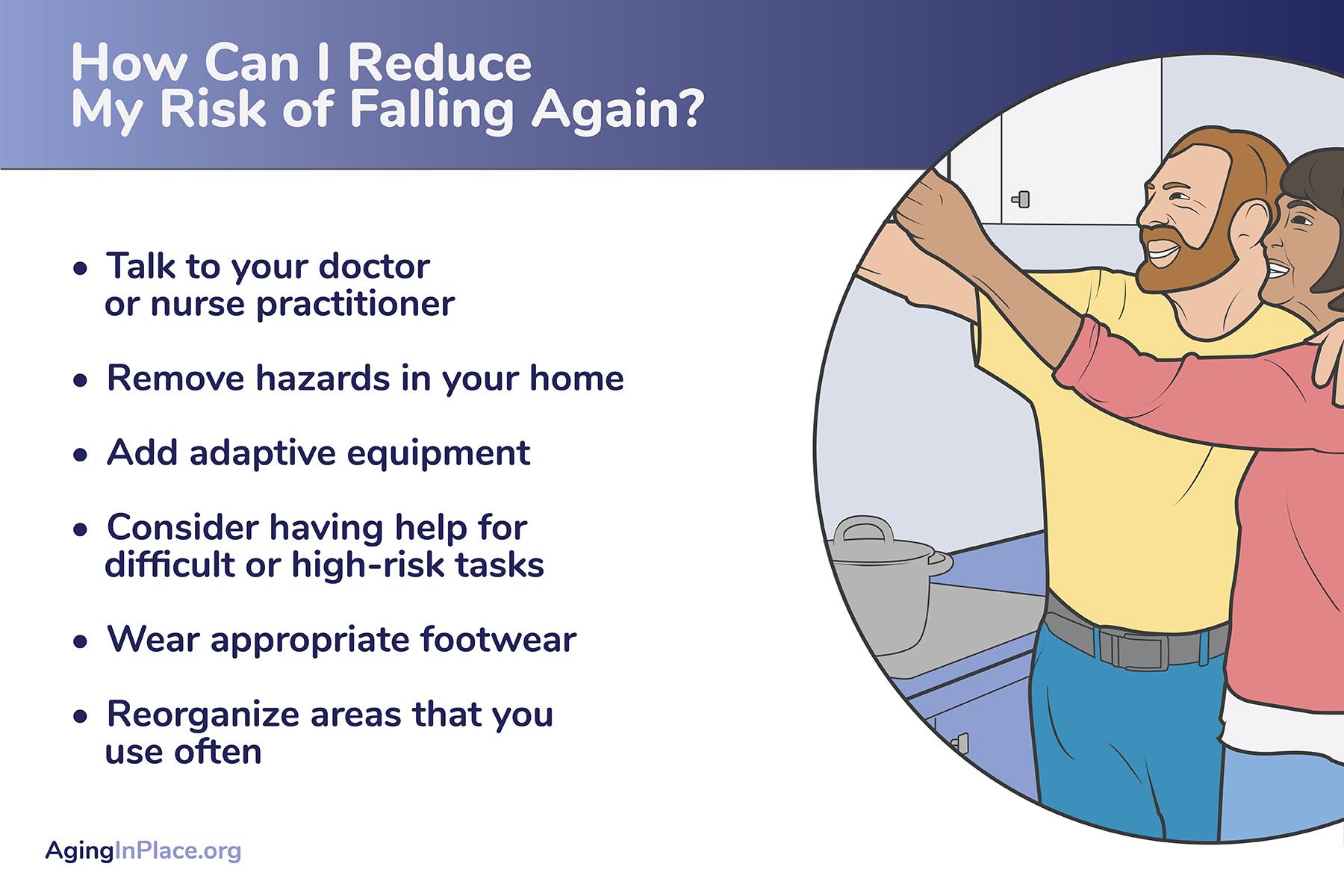
How Can I Reduce My Risk of Falling Again?
- Talk to your doctor or nurse practitioner. The first thing you should do if you’ve fallen is to consult with your physician or health care provider to make sure that it wasn’t due to any physical problems or health conditions. Your doctor can help you to identify new or worsening symptoms, develop treatment plans, and assess your medications to rule out negative side effects from polypharmacy.
- Remove hazards in your home. Keep area rugs limited to low-traffic areas, and move small tables, lamps, or any other smaller furniture away from paths you usually take while moving through your home.
- Add adaptive equipment. If there are any areas where you have to walk a significant distance, installing grab bars on walls can provide stability as you move throughout your home. Grab bars are also good additions to bathrooms and kitchens where floors can be slippery. You can also make bathrooms safer by installing raised toilets to reduce the distance you have to sit down and stand up, and shower chairs to eliminate the need to stand while you shower.
“This is one of the biggest things I run into in practice: people’s hesitancy to ask for or accept help with tasks around the house,” said Norman. “I’ll often ask people open-endedly: ‘Is it better to accept some help now before there’s an accident or after the accident has already occurred?’ Before a fall or accident, you have lots of choices. After a fall or accident, you may not have as many choices.”
4. Consider having help for difficult or high-risk tasks. You may not want or need full-time help at home, but it’s a good idea to consider occasional help during activities like bathing, cooking, or cleaning. This help can be from a friend, a family member, or even a home care agency.
5. Wear appropriate footwear. A sturdy, closed-toe shoe that fits properly is a good way to enhance your stability. If you’d rather not wear shoes at home and prefer socks, make sure that your socks have slip-resistant texturing on the bottom.
6. Reorganize areas that you use often. Kitchens, bathrooms, and bedrooms should be organized to make sure that everything you need is within reach and easily accessible without climbing or reaching.
Bottom Line
If you or a loved one has fallen and are worried about next steps and your future at home, a fall is not the end of your independence. Taking the steps to identify causes, manage your health and medications, and eliminate hazards in your home can keep you on track to age in place for many years to come.